
Nobody wakes up in the morning and decides to get cancer. And yet, quietly, invisibly, millions of Americans are making dozens of small decisions every single day that inch them closer to a diagnosis they never saw coming. The cigarette in the car. The soda with lunch. The couch after dinner. The job so stressful it keeps cortisol perpetually spiked. None of it feels dangerous in the moment. All of it adds up.
Cancer has long carried the reputation of being a bolt from the blue — a cruel genetic lottery, a matter of bad luck. And while genetics do play a role, the science tells a far more complicated, and ultimately more hopeful, story. According to the American Cancer Society, roughly 42% of all cancer cases in the United States are attributable to modifiable risk factors. That’s nearly half. Things that, in theory, we can change.
What Stats says....?

So what does a “cancer lifestyle” actually look like? Spoiler: it looks a lot like modern American life. And understanding that is both sobering and strangely liberating.
The Lifestyle Shift in Modern America
Over the past few decades, the American lifestyle has changed dramatically. Technological convenience, fast food culture, and sedentary work environments have transformed how people eat, move, and live.
Several trends have become common:
Processed and ultra-processed food consumption
Sedentary desk jobs and reduced physical activity
Rising obesity rates
Chronic stress and sleep deprivation
Alcohol consumption and smoking habits
These lifestyle patterns collectively influence cancer risk in powerful ways.
Tobacco: The One We Already Know — and Still Don't Fix
We’ve known since 1964 that smoking causes lung cancer. That’s over sixty years of knowing — and yet tobacco remains the single largest preventable cause of cancer death in America, responsible for nearly 30% of all cancer deaths. Lung cancer still kills more Americans each year than breast, prostate, and colon cancer combined.
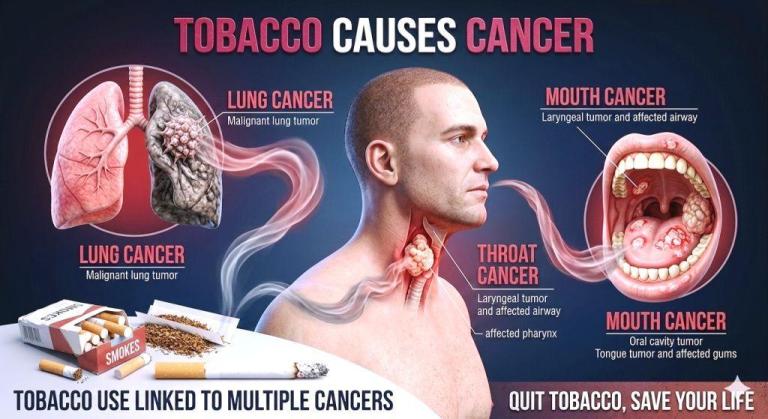
But here’s what many people still don’t fully grasp: smoking doesn’t only cause lung cancer. It’s linked to cancers of the mouth, throat, esophagus, stomach, pancreas, kidney, bladder, cervix, and more. If tobacco were a new product introduced today, it would never see a store shelf. The fact that it’s legal, marketed, and woven into cultural history has made it uniquely difficult to eradicate.
And then there’s vaping — sold to a generation of teenagers as the “safer” alternative. The jury is still out on long-term cancer risk from e-cigarettes, but early signals are not reassuring. Several vaping compounds have shown DNA-damaging effects in lab studies. The American Cancer Society has been unequivocal: there is no safe form of tobacco or nicotine delivery.

What America Eats — and What It's Doing to Our Cells
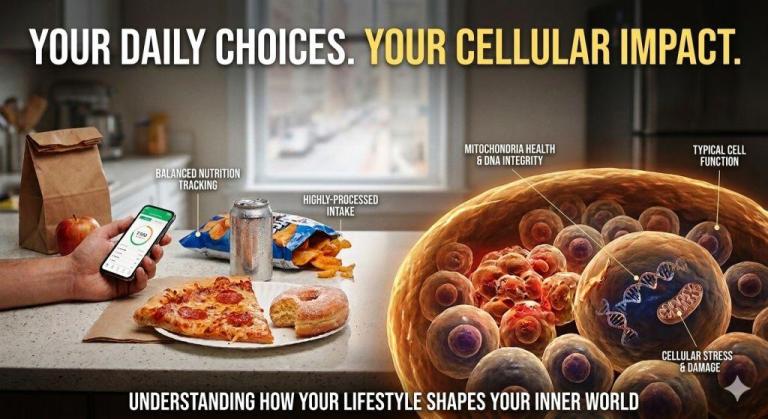
Walk through any American grocery store and you’re essentially navigating a war between two food systems. On one side: the produce aisle, the legumes, the whole grains — foods that have existed for millennia and that the human body recognizes intimately. On the other: the ultra-processed center aisles, engineered for maximum palatability and minimum satiety, loaded with refined sugars, industrial seed oils, and preservatives.
Most Americans spend most of their food budget in that second world. And the research is increasingly clear about the consequences. Ultra-processed food consumption has been linked in multiple large-scale studies to elevated cancer risk — particularly colorectal cancer, which has been rising sharply in Americans under 50, a trend that has genuinely alarmed oncologists.
Red and processed meat deserve special mention. The World Health Organization classifies processed meats — deli slices, hot dogs, bacon — as Group 1 carcinogens: the same category as tobacco smoke. Red meat is Group 2A, meaning it probably causes cancer. These classifications don’t mean a hamburger is as dangerous as a cigarette, but they do mean the evidence of risk is real, consistent, and worth taking seriously at your dinner table.
➦ Colorectal cancer risk rises significantly with regular processed meat consumption.
➦ Alcohol is directly linked to at least 6 types of cancer, including breast and liver.
➦ Obesity is a known risk factor for at least 13 different cancer types.
➦ Fiber-rich diets are strongly associated with reduced colorectal cancer risk.
➦ Cruciferous vegetables — broccoli, cauliflower, kale — contain compounds that support DNA repair.
And alcohol? It may be the most socially normalized cancer risk factor in America. Drinking is woven into celebration, grief, stress relief, and socializing. But alcohol is a Group 1 carcinogen too — linked to cancers of the breast, colon, liver, esophagus, and mouth. Crucially, the risk isn’t just for heavy drinkers. Even light to moderate drinking raises breast cancer risk, which catches many women completely off guard.
Sitting Is the New Smoking — And America Can't Stand Up

When researchers began calling physical inactivity “the new smoking,” it was partly provocative, but the underlying science is serious. Regular physical activity is associated with reduced risk for at least 13 types of cancer, including breast, colon, endometrial, bladder, kidney, and gastric cancers. The mechanisms are multiple: exercise reduces circulating insulin and estrogen, decreases inflammation, improves immune function, and maintains healthy body weight.
The average American sits for roughly 9 to 10 hours a day. We sit to commute, work, eat, and relax. Our built environment — suburban sprawl, car-dependent cities, desk-bound jobs — makes sedentary behavior the default rather than the exception. This isn’t purely a personal failure; it’s partly an infrastructure problem. But that doesn’t make the biological consequences any less real.
The good news is that you don’t need to become a marathoner. Studies consistently show that even modest exercise — about 150 minutes of moderate activity per week, or roughly 22 minutes a day — meaningfully reduces cancer risk. Walking counts. Gardening counts. Dancing in your kitchen at midnight absolutely counts.
The Obesity Connection
Excess body weight is now the second leading preventable cause of cancer in the US, after tobacco. Fat tissue — particularly visceral fat around the abdomen — is metabolically active. It releases hormones, growth factors, and inflammatory molecules that can promote tumor growth. Maintaining a healthy weight through diet and exercise isn’t just about appearance; it’s one of the most powerful cancer-prevention levers a person has.
Stress, Sleep, and the Invisible Carcinogens of Modern Life
Here’s a dimension of the lifestyle-cancer conversation that rarely gets the attention it deserves: the chronic, grinding, unrelenting stress that has become the ambient soundtrack of American life. Deadlines, debt, political anxiety, social media comparison, sleep deprivation — these aren’t just bad for your mood. They dysregulate the immune system, drive chronic inflammation, and create hormonal environments that cancer cells find particularly hospitable.
The research on sleep is especially compelling. People who chronically sleep fewer than six hours per night show altered immune function and higher rates of certain cancers. Night-shift workers — nurses, factory workers, truck drivers — have elevated cancer risk significant enough that the WHO has classified night-shift work as a probable carcinogen. Sleep is when the body conducts cellular repair, clears metabolic waste, and resets immune surveillance. Shortchange it, and you shortchange your body’s cancer-fighting machinery.
Environmental Exposures: The Risks You Didn’t Choose
Not all lifestyle risk factors are truly individual choices. Environmental exposures — radon in the home, air pollution, occupational chemical exposure, contaminated water — affect cancer risk in ways that map closely onto socioeconomic and racial lines in America. Low-income communities and communities of color bear disproportionate environmental cancer burdens due to proximity to industrial sites, older housing stock, and reduced access to safe spaces for exercise.
Radon gas alone — colorless, odorless, seeping up through soil into basements across America — is the second leading cause of lung cancer in the US, responsible for approximately 21,000 deaths annually. Most homeowners have never tested for it. A $15 test kit from any hardware store can genuinely save your life. That disproportion between risk and awareness is, frankly, remarkable.
“Cancer is not inevitable. It’s a conversation between your genome and your environment — and you have more say in that conversation than most people realize.”
— Dr. Otis Brawley, Bloomberg Distinguished Professor, Johns Hopkins University
What Actually Changes Risk — A Realistic Picture
Here’s where honesty matters most. This isn’t a story about perfection. Nobody eats perfectly, exercises daily, sleeps eight hours, and lives in a stress-free environment. The goal isn’t a flawless lifestyle — it’s a meaningfully better one. Risk reduction, not risk elimination.
➦ Quitting smoking at any age dramatically reduces lung and other cancer risks within years.
➦ Reducing alcohol consumption meaningfully lowers breast and colorectal cancer risk.
➦ Losing even 5–10% of body weight if overweight improves cancer-related biomarkers.
➦ Getting screened on schedule catches cancers early, when they are most treatable
➦ Testing your home for radon is cheap, easy, and potentially life-saving.
➦ Daily broad-spectrum SPF 30+ sunscreen substantially cuts skin cancer risk.
Quitting smoking — even in middle age — begins reducing cancer risk almost immediately. Within ten years of quitting, lung cancer risk drops by about half. Reducing alcohol lowers breast cancer risk. Adding fiber to your diet shifts your gut microbiome and colon cancer risk within weeks. These are not distant, abstract benefits. They are near-term, measurable biological shifts happening in your body right now.
Quitting smoking — even in middle age — begins reducing cancer risk almost immediately. Within ten years of quitting, lung cancer risk drops by about half. Reducing alcohol lowers breast cancer risk. Adding fiber to your diet shifts your gut microbiome and colon cancer risk within weeks. These are not distant, abstract benefits. They are near-term, measurable biological shifts happening in your body right now.

