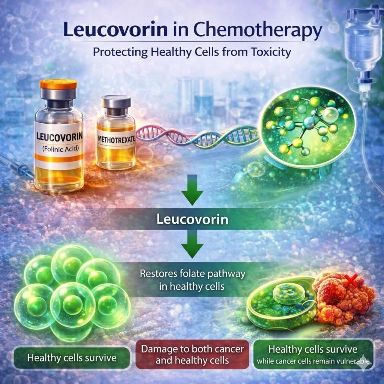
Leucovorin is a widely used medication in oncology and clinical medicine that plays a unique dual role: it can protect healthy cells from chemotherapy damage while also enhancing the effectiveness of certain anticancer drugs. Known scientifically as folinic acid, leucovorin is a biologically active form of vitamin B9 used in cancer therapy, toxicology, and hematology.
This article explains:
- What Leucovorin is, how it works.
- Its clinical uses.
- Statistics, side effects.
- Its growing role in modern medicine.
⚫ What Exactly is Leucovorin?
Leucovorin — also known as folinic acid or citrovorum factor — is the pharmacologically active form of folic acid. Unlike folic acid, it does not require enzymatic conversion by dihydrofolate reductase (DHFR) to become active. This single biochemical distinction makes it extraordinarily useful in clinical practice.
Chemically, it is 5-formyl tetrahydrofolic acid. It acts as a carrier of one-carbon units critical for nucleotide biosynthesis and amino acid metabolism. When used therapeutically, it either potentiates chemotherapy or rescues normal cells from drug toxicity — depending entirely on the clinical context.

⚫ Mechanism Summary:
Step-by-step process
- Methotrexate blocks folate metabolism.
- DNA synthesis stops in rapidly dividing cells.
- Leucovorin provides a usable form of folate.
- Healthy cells recover and resume normal function.
In contrast, when leucovorin is combined with fluorouracil (5-FU), it enhances the anticancer effect by stabilizing the drug’s interaction with the enzyme thymidylate synthase.
This dual mechanism makes leucovorin extremely valuable in oncology.
⚫ Main Medical Uses of Leucovorin:
1. Rescue Therapy After Methotrexate:
High-dose methotrexate is commonly used to treat cancers like osteosarcoma. However, it can cause severe toxicity. Leucovorin is administered after chemotherapy to reduce toxicity and protect healthy tissues.
2. Treatment of Colorectal Cancer:
Leucovorin is frequently combined with fluorouracil (5-FU) in colorectal cancer treatment.
One widely used regimen is the FOLFOX protocol, which includes:
- Leucovorin
- Fluorouracil (5-FU)
- Oxaliplatin
This combination increases chemotherapy effectiveness and improves survival outcomes.
3.Treatment of Megaloblastic Anemia:
Leucovorin can treat megaloblastic anemia caused by folate deficiency, particularly when oral folic acid cannot be used.
4. Antidote for Drug Toxicity:
Leucovorin is also used to counteract toxic effects of folate-antagonist drugs, including:
- Methotrexate overdose
- Trimethoprim
- Pyrimethamine
5. Emerging Neurological Uses:
Recent research has explored leucovorin for cerebral folate deficiency, a rare disorder that can cause neurological symptoms resembling autism.
However, evidence remains limited and more clinical trials are needed.
⚫ Clinical Statistics and Data:
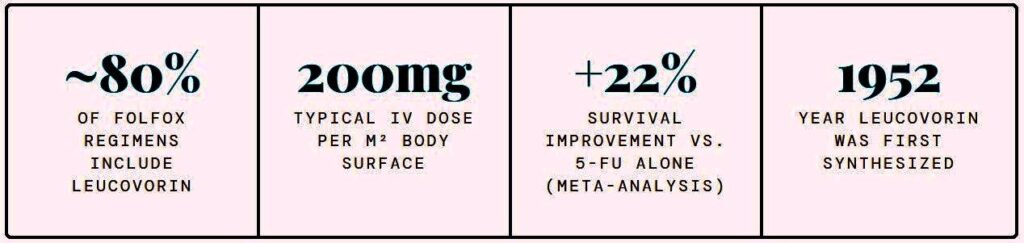
The importance of leucovorin becomes clear when examining cancer treatment statistics.
Global Colorectal Cancer Burden
- Over 1.9 million new colorectal cancer cases occur globally each year.
- It is the third most common cancer worldwide.
Leucovorin-based chemotherapy regimens remain a cornerstone of treatment.
Methotrexate Toxicity
High-dose methotrexate can cause:
- Bone marrow suppression
- Kidney injury
- Severe gastrointestinal toxicity
Leucovorin rescue therapy significantly reduces these complications, making aggressive chemotherapy possible.
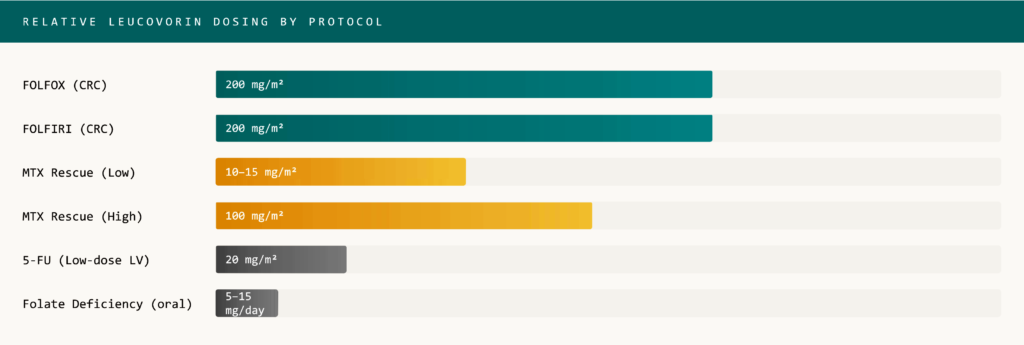
⚫ Dosing Regimens at a Glance:
Leucovorin dosing varies significantly based on context. The chart below illustrates relative dose ranges across major clinical protocols (IV administration, normalized to 200 mg/m² base dose).
⚠ Clinical Note
In methotrexate rescue protocols, leucovorin must not be given simultaneously with methotrexate. Timing — typically 24 hours post-MTX — is critical. Inadequate leucovorin rescue or late initiation is associated with significantly increased treatment-related mortality.
⚫ Safety Profile & Side Effects:
Leucovorin is generally well-tolerated when used correctly. Its adverse effect profile is modest compared to most oncologic agents, though clinicians should remain vigilant for the following:

⚫ The Evidence: What Studies Tell Us
Leucovorin’s integration into colorectal cancer treatment has been validated by decades of rigorous research. A landmark 1992 meta-analysis by the Advanced Colorectal Cancer Meta-Analysis Project (N=1,381) found that leucovorin modulation of 5-FU improved tumor response rates from 11% to 23%, though overall survival benefit was more modest.
More recently, the MOSAIC trial demonstrated that FOLFOX4 — which includes leucovorin — reduced the risk of disease recurrence by 23% compared to 5-FU alone in stage III colon cancer (HR 0.77; p=0.002). The 10-year follow-up confirmed durable overall survival benefit (HR 0.80; p=0.029).
In the pediatric oncology setting, leucovorin rescue protocols after high-dose methotrexate have made it possible to safely administer MTX doses as high as 12 g/m² in osteosarcoma and ALL — doses that would otherwise be prohibitively toxic.
⚫ The Bottom Line:
Leucovorin exemplifies how supporting agents — not just frontline cytotoxics — define the safety and efficacy of modern chemotherapy. It simultaneously amplifies the cancer-killing power of 5-FU and provides a biological safety net when methotrexate threatens to overwhelm normal tissue.
As precision oncology continues to evolve, leucovorin remains a cornerstone of combination regimens in colorectal, gastric, and hematologic cancers. Its dual role as potentiator and rescuer is nearly unparalleled in the pharmacopeia. Clinicians who understand its mechanisms and indications hold a powerful tool — one that has quietly saved countless lives since 1952.
Understanding leucovorin is not merely pharmacology — it is understanding the art of chemotherapy itself.